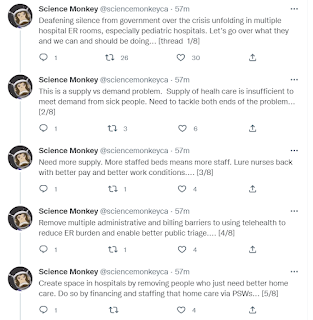
I was reading this tweet run:
And it made me think of the time this month that there were reports of the 911 number in Toronto asking for call back numbers after a medical emergency. Even if overstated, it really does bring to light the key problem with telehealth -- that call center culture is famously customer-hostile.
A number of years back I had a problem with my cable company. Like many foolish persons, I called the cable company and spent 2 hours on hold. After I was told that nothing could be done, I asked if there was anybody I could speak with that had more authority to deal with the issues. I was then placed on hold again. Several hours later a message played saying that the call center was closing and disconnected me. This was an infuriating experience and there was simply no accountability even possible. So the next day I made the long trek to the customer service center, waited in line for about an hour, and then had the problem actually fixed. No part of this experience made me like the company more, but the call experience was terrible.
Recently, I have been constantly hearing "call volumes are unexpectedly high" recordings every time I call a place like a bank or the University travel agent. As a person who once worked in customer service telemarketing call volume forecasting, I even tried times and days that are notoriously light for call volume. No luck.
So the central challenge of telehealth is how to break with the cost-cutting culture that values customer wait times at zero (or even seems to see them as a good thing). You can only redirect from the Emergency Room via telehealth triage if it is relatively quick (let us say an hour, maximum). Because you get no triage credit at the ER for having called telehealth, so if the answer is "go to the ER" but you have lost 4 hours on the phone then that is going to quickly teach everyone not to call telehealth lines.
With pediatric ERs reporting wait times as long as 15 hours, you can see the value of telehealth if it can keep children out of the queue and free up capacity. But that really requires that it be agile (why wait 4 hours as a prelude to waiting 15) and able to do things like prescribe. I know that RSV is an atypically severe phase, but at some point the default needs to be that there are a lot of respiratory viruses running around and we should plan around that.
That gets me to my last pet peeve about telemedicine, which that you need to be able to provide helpful interventions. In a recent covid burst, I had a family member use a telemedicine provider to ask about paxlovid only to be told that it could not be prescribed by phone but that it required an in-person visit. Yes, the plan really was for the infectious person to sit in the waiting room of a walk-in clinic for hours so that the prescription could be written by a person able to see the patient. Now, whether or not treating covid with paxlovid was a good idea is a different question but the issue was that these policies make calling first seem like a bad plan, as you waited hours for an appointment making it much less likely that you can successfully get seen at a walk-in clinic with a time-sensitive health issue.
Which is the opposite of what you want people to do, frankly.
Without solving these cultural issues of how we treat in-calls and how we treat patients, we are not going to be able to really move the demand side for ERs.
No comments:
Post a Comment